How To Manage Respiratory Arrest

Respiratory arrest involves the cessation of breathing and it can happen for a number of different reasons.
Regardless of the underlying cause, however, it is almost always a life-threatening experience that requires immediate medical attention.
When someone goes into respiratory arrest, their vital organs cease receiving oxygen.
If not property treated, the patient may suffer cardiac arrest and/or possible brain damage within just minutes of onset.
In some instances, impending respiratory arrest may be identifiable before it occurs.
One of the most common signs to watch for is labored breathing in which the patient has to work increasingly hard to take a sufficient breath.
When this occurs, the patient will ultimately deplete their reserves of air and be unable to maintain the extra effort that is required to breathe sufficiently.
Without prompt and effective intervention, this will most likely lead to respiratory arrest.
Additional early signs of respiratory arrest include, but are not limited to: gasping for air, cyanosis, paradoxical breathing movements and intercostal retractions.
Some sufferers of respiratory arrest also experience mental confusion or become markedly sleepy.
This is due to the hypoxia and increased levels of carbon dioxide.
In most instances, if the signs of impending respiratory failure are identified right away, treatment can be administered immediately, thereby preventing the onset of total respiratory arrest.
Recalling the Basics

For those first on the scene of a respiratory arrest, the situation can be stressful.
As a result, it can be easy to forget the basics.
Take a deep breath and try to focus.
The first thing you’ll need to do is assess the patient’s responsiveness.
If the person is unresponsive or minimally responsive with abnormal breathing or gasping, open his or her airway and start manually ventilating (Keeping in mind not to cause excessive ventilation).
If you are working within a hospital setting and a code blue has not yet been activated, now is the time to do so.
A pulse may initially be present, however, should the patient develop cardiac arrest you must be prepared to begin chest compressions immediately.
Open the victim’s airway and deliver positive pressure ventilation using a bag mask.
In most situations, you will be able to open the airway using the head-tilt, chin-lift method.
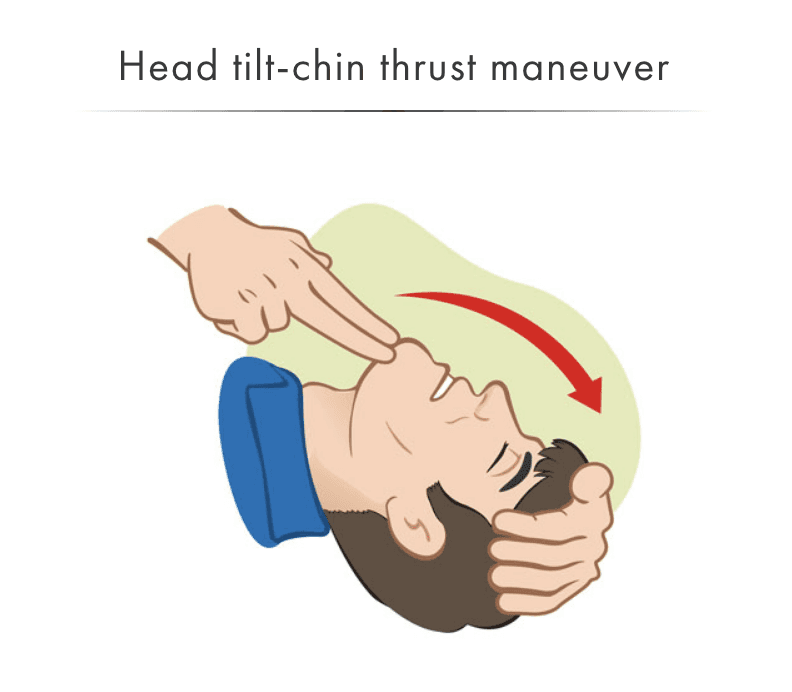
An exception would be made in the event that the patient has suffered a neck or spinal cord injury.
In a hospital setting, make sure that the bag mask you are using is attached to the oxygen flow meter and that the oxygen is turned all the way up.
To prevent the tongue from blocking the airway, the use of an oral airway can be helpful.
This should only be used, however, in patients that are unconscious, since an oral airway will cause gagging.
In patients that are fully or semi-conscious, opt instead for a nasal airway.
When you are holding the bag mask, make sure to create a tight seal over the patient’s nose and mouth.
Be careful not to ventilate too quickly.
Often times – especially in situations that are stressful – adrenaline tends to take over.
If you ventilate too fast, you risk hyperventilating the patient.
Remember that ventilating too quickly or using a tidal volume that is too large can decrease cardiac output, increase intrathoracic pressure, decrease venous return to the heart and result in gastric distension.
Breaths in for adult respiratory arrest patients should be delivered at a rate of 10 to 12 per minute (or one breath every five to six seconds).
If you notice the patient’s chest rising with each breath, you’ll know you are delivering adequate ventilation.
As you continue to bag, you should also attach a pulse oximeter to monitor the patient’s oxygen level and heart rate.
Advanced Airway Management
After delivering positive pressure ventilation using a bag mask, the patient may begin spontaneously breathing on his or her own.
If this happens, verify that the breathing is adequate.
Then administer supplemental oxygen and continue to monitor.
If independent breathing does not occur, the patient may require intubation.
Bag mask ventilation should continue as the intubation equipment is prepared.
Prior to intubation, the patient’s mouth and oropharynx may need to be suctioned in order to remove any secretions and gain adequate visibility of the vocal cords.
Confirmation of successful intubation of the trachea may be initially verified by the rising of the patient’s chest.
Additionally, an end tidal C02 device should be placed to indicate the presence of carbon dioxide during exhalation.
To further confirm proper tube placement, a chest x-ray should be performed as soon as possible.
At this point, you will need to place the patient on a mechanical ventilator.
Identify and Address the Underlying Cause
Respiratory arrest can occur for a wide variety of reasons.
For instance, an overdose of drugs can result in a depressed nervous system and ultimately lead to respiratory failure.
Additionally, some neuromuscular conditions can cause severe fatigue, which can eventually result in the cessation of breathing.
Strokes, metabolic disorders and airway obstructions can also lead to respiratory arrest.
Being aware of the patient’s medical history, their main complaint and any medications they may be taking can all be helpful in determining the underlying cause of respiratory failure.
Absent this information, certain diagnostic blood tests, such as complete blood count (CBC) and measuring arterial blood gases and electrolytes may provide clues as to what is causing the patient to experience respiratory arrest.
An x-ray of the chest should also be performed.
Once all of the puzzle pieces begin falling into place, a definitive diagnosis can be reached and effective treatment can be administered.
Conclusion
Managing respiratory arrest properly can literally save someone’s life.
That’s why it’s so important to remain calm, get back to basics and know what steps to take to get the situation under control as quickly and effectively as possible.
Are you interested in learning more about this or other emergency resuscitation techniques?
Our online ACLS course is the quickest, most affordable and convenient way to do so. Click here below to learn more or to sign up today!
